MAINE, USA — Throughout the COVID-19 pandemic, other public health challenges raged on. Substance use in Maine surged and obesity rates continued to tick upward. Fatal drug overdoses in the state set records in 2020 and 2021, and are on track to do so again.
Smoking rates have fallen but Maine still has higher rates than the national average. Vaping skyrocketed before the pandemic and overall tobacco use has increased among youth.
Youth rates of smoking, drinking and vaping all declined during the pandemic. But public health experts cautioned that these changes could be temporary, due to lack of access to substances during COVID-19 orders to stay at home.
In sum, many indicators of health in Maine worsened during Gov. Janet Mills’ term, but came as she and leaders across the world dealt with the worst public health crisis in a century — a worldwide pandemic that claimed more than 2,600 lives in Maine and more than a million nationally. And, data shows, many of the same indicators also worsened under her lead challenger, Republican Paul LePage, who was governor from 2011-19.
Now, as Maine enters its third pandemic winter, public health experts are struggling to assess and address the other health challenges that continue alongside the stubborn struggles with COVID-19.
Under Mills, the Maine Center for Disease Control and Prevention is restructuring its approach to prevention work around obesity, tobacco and substance use. Prevention funds will flow directly to the eight public health districts rather than statewide organizations like MaineHealth.
The move will create more local control and is intended to bolster the local public health infrastructure in a state unusual for its lack of county public health departments.
Public health experts said this change has been in the works for a while and is a step in the right direction, but more work needs to be done to build up local public health.
Opioid use in Maine increased under both the LePage and Mills administrations.
After climbing for years, fatal opioid overdoses dipped to 354 in 2018 before ticking up again. Then in 2020, the first year of the pandemic, drug deaths increased 33% over the previous year to 504.

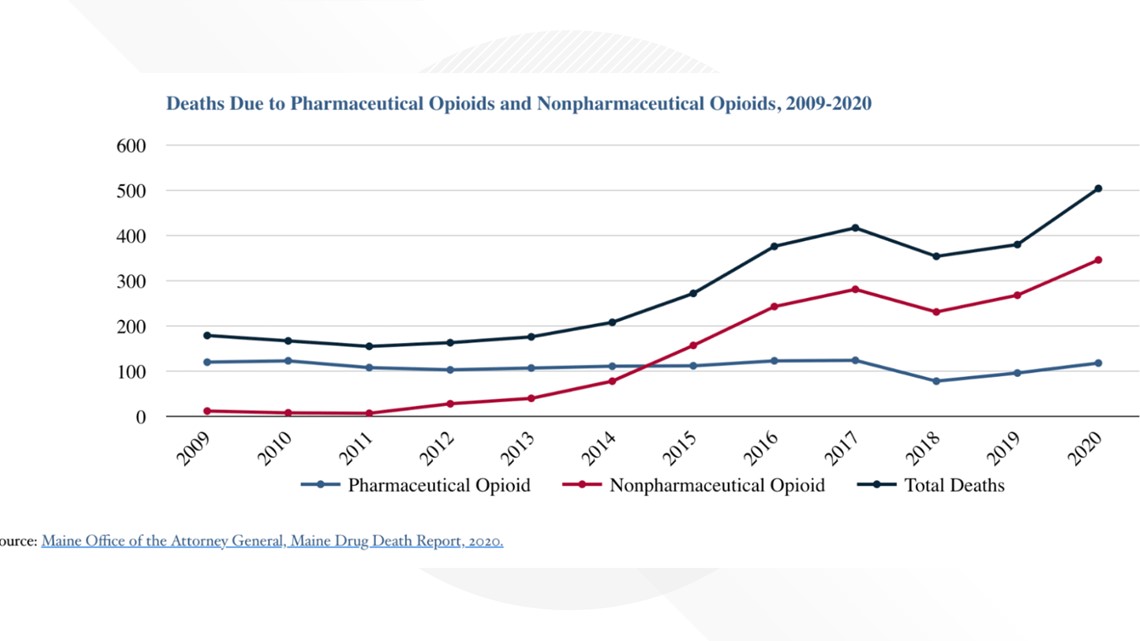
This year, fatal overdoses are on track to surpass last year’s record number. There were nearly 800 more overdoses — fatal and nonfatal — as of August compared with the same period last year, according to the monthly overdose report funded by the Maine Office of the Attorney General and the Office of Behavioral Health.
The recent surge could be attributed, at least in part, to the mental health crisis spurred by the pandemic and a rise in fentanyl, which was involved in an estimated 77% of Maine drug deaths.
Tobacco use among youth increased from about 11% in 2019 to 20% last year, according to the Maine Integrated Youth Health Survey. This could be because the question in 2019 did not include electronic cigarettes, which was on the rise before the pandemic. Youth vaping nearly doubled between 2017 and 2019.
Youth drinking has declined for years under both governors. In 2011, when LePage took office, 28% of Maine high school students reported currently drinking alcohol. That dropped to about 23% by the time Mills took office in 2019. Last year the rate was 19%.
While vaping skyrocketed in the years leading to the pandemic, traditional cigarette smoking dropped in Maine from 23% in 2011 to less than 16% last year.

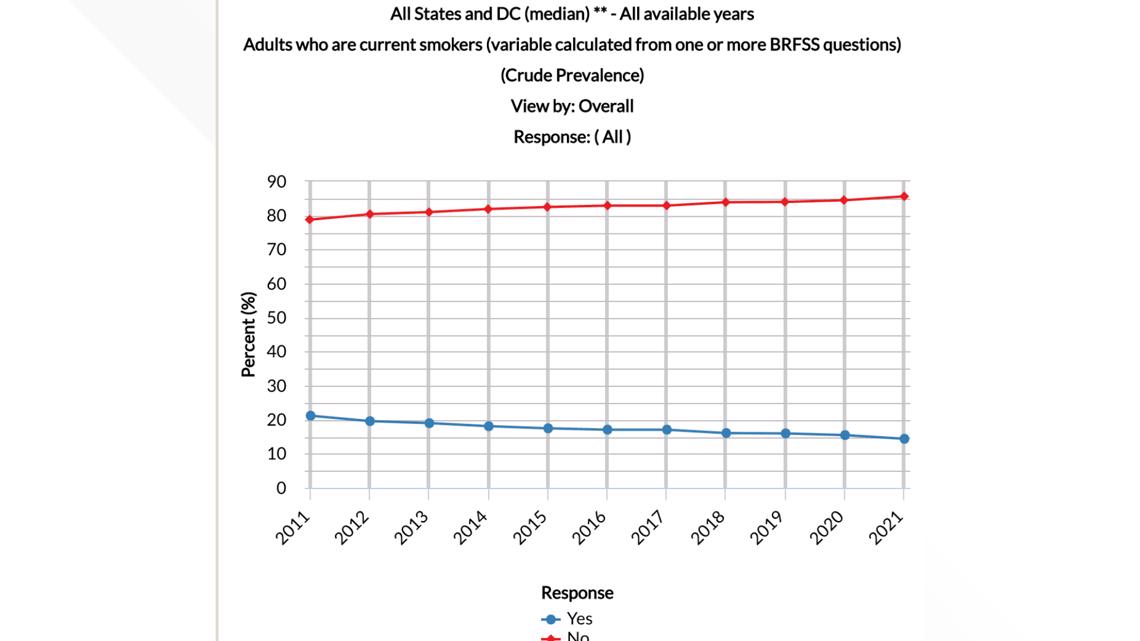
Deborah Deatrick, retired senior vice president for community health improvements at MaineHealth, attributed the lowered smoking rates to Maine’s success with treatment, prevention and policy. She pointed to laws requiring smoke-free restaurants and indoor spaces, tighter vaping restrictions, and better access to treatment methods like nicotine replacement therapy and counseling.
“In terms of tobacco and obesity, we know what to do. We know what works. We have some policies and programs and strategies that we know have borne results,” Deatrick said. “It’s really a matter of keeping our pedal to the metal and keeping on with what we’re doing collectively in the public and private sector.”
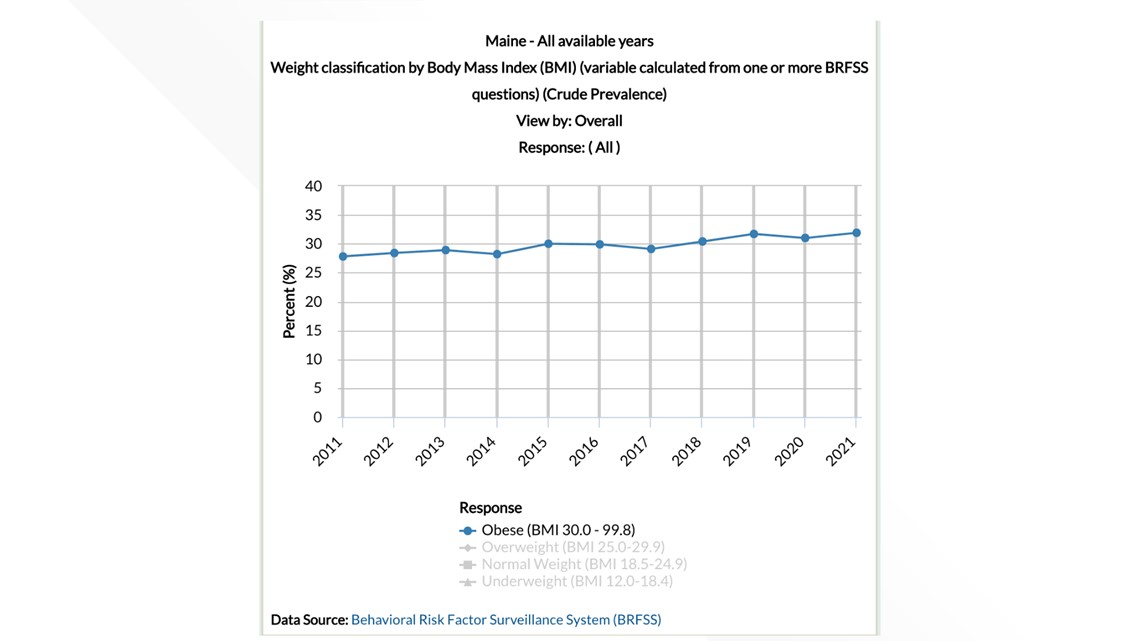
However, obesity has continued to prove challenging. The number of adult obese Mainers increased threefold since the early 1990s, said Rebecca Boulos, executive director of the Maine Public Health Association.
Last year, nearly 32% of Mainers were obese, according to the U.S. CDC. The national rate of obesity last year was 33.9%.
When LePage took office in 2011, Maine’s obesity rate was 27.8%. When Mills took office in 2019, it was 31.7%.

People who are lower income, have less education, are racial and ethnic minorities, or live in rural areas are at higher risk of obesity, Boulos said. Many risk factors are shared with tobacco and substance use.
“Obesity is a very complex chronic disease,” Boulos said. “It’s a constellation of factors. The determinants of obesity have to do with genetics and access to safe places to recreate, and affordable healthy foods.”
Social and physical environments, biological and genetic factors, mental health, personal views, health insurance coverage, socioeconomic status, and product accessibility, availability and price all make prevention work complex, said Robert Long, spokesman for the Maine CDC.
“Maine CDC is committed to continuing to work with partners across the state to address these issues as part of an ongoing and collaborative effort to improve the health and well-being of Maine residents,” Long said.
One way the Maine CDC is trying to address health problems is to restructure the public health bureaucracy and put prevention money directly in the hands of local agencies.
The Maine CDC will distribute funds through the state’s eight public health districts to contract with local groups providing substance use, tobacco use and obesity prevention work.
This will “allow more funding to go directly toward prevention services,” Long said. Maine CDC will work with awarded bidders to create a plan based on the priorities identified in conversations with local stakeholders and community members.
Previously the Maine CDC distributed funds to a larger contractor, like the University of New England or MaineHealth, which then distributed the funds to subcontractors in local communities.
The change could create a more “regional approach” to the prevention work in a rural state that doesn’t have county-level public health departments, said Bridget Rauscher, who manages prevention programs for tobacco, obesity and substance use for the Portland Public Health Division.
“I think the purpose is to focus on the region that you’re serving so it’s more centralized, so on-the-ground work can be more impactful for the community,” Rauscher said. “The way it’s broken into public health regions aligns with infrastructure at the state level, and can allow regions to tailor work to the needs of the community.”
Rauscher said she is optimistic the outcomes will improve because the prevention measures will better reflect the community being served. For example, she said, some parts of the state may not need Portland’s level of funding for health equity strategies around language barriers, whereas Portland may face fewer transportation barriers than more rural communities.
Rauscher works with schools and early childhood education to teach skills that build resilience and confidence.
“We’re teaching kids to stand up for themselves, to think critically and independently, and build self-esteem,” Rauscher said. “We’re not just saying, ‘Don’t smoke. Don’t use drugs.’ It’s skill-building. Lifelong skill-building.”
Boulos, with Maine Public Health Association, said the change brings more focus on prevention. Prevention doesn’t always get as much attention or focus as treatment because it’s hard to quantify. But one estimate, from Trust for America’s Health, found that for every dollar spent in chronic disease prevention programs in Maine, the state gets a $7.50 return on its investment within five years.
This new approach will build on existing relationships and community partnerships, regardless of who is governor next year, Boulos said.
“Those (partnerships) transcend administrations,” she said. “They’ve been building for decades and will continue to build past the next four years..”
Deatrick, who retired from MaineHealth and is now a public health consultant, said historically there haven’t been enough groups on the ground doing outreach or funding for the work.
“The concept is a really good one. It’s something public health has been talking about for decades, which is building local or regional public health infrastructure, which for the most part we don’t have in Maine,” Deatrick said. “From a general standpoint I think it’s great that Maine CDC is building local regional public health infrastructure.”
But there’s still a place for public health and private health organizations to work together, Deatrick said. The approach going forward should be a partnership between public and private.
For example, the money distributed by Maine CDC for tobacco prevention comes from state and federal funding but it supports work done in the private sector, Deatrick said.
“It’s symbiotic. You scratch my back and I scratch yours. You need both. The public sector can only do so much,” Deatrick said. “What the Maine CDC is trying to do now is go a step further in bridging that gap between the government and local regions of the state by putting some money into building some local infrastructure.”
As governors, Mills and LePage had different philosophies on public health. Under LePage, the number of filled positions in the Maine CDC shrunk from 418 to 333 in January 2019. Under Mills, 404 positions are filled today, according to Scott Ogden, spokesman for the Mills reelection campaign.
In particular, the public health nursing program shrunk under LePage from more than 50 positions to fewer than 20 at one point. Public health nurses with the Maine CDC are responsible for home visits with expectant moms and new infants, and serve as a local source of health information in their community.
LePage previously told The Maine Monitor in March that the public health nurse program needed more oversight and a better reporting structure. He promised at the time to fill all vacant positions and fully fund the program if reelected.
“I’m a big believer that if you’re going to hire people, they have to be effective and they have to optimize their skill level to help society,” LePage said at the time. “These are public health nurses being paid by the public and the public has a desire to get the proper services.”
He said he wants to eradicate poverty, domestic violence and opioid addiction through programs that help people help themselves, not by “giving them everything and letting them go to their own devices.”
A spokesman for LePage did not provide responses from the former governor for this story.
LePage previously has supported some investment into opioid treatment as well as advocated for a detoxification center, but he vetoed legislation that expanded access to naloxone, the lifesaving narcotic that can reverse an overdose. He wrote in his veto message that “Naloxone does not truly save lives; it merely extends them until the next overdose.”
LePage also has criticized Mills’ mandate that all healthcare workers get vaccinated against COVID-19.
LePage’s attitude toward public health seemed to imply that “it isn’t all that important and we’ll let the community take care of this,” Deatrick said.
In response to shrinking public health positions under LePage, the private healthcare sector started funding its own public health programs, said Deatrick, who was with MaineHealth for 20 years.
Deatrick said most people in public health seem to share her concerns about LePage.
“You may find somebody who says (LePage) did a great job with X, but I couldn’t think of a public health issue where I would give him a positive grade,” Deatrick said.
In response to the substance use crisis, Mills expanded prevention, treatment and recovery programs, with plans to continue expanding, Ogden said. He added that Mills expanded Medicaid, which resulted in more than 22,000 Mainers receiving substance use disorder treatment.
Mills also signed a law banning vaping and tobacco products on school grounds and buses, supported $7 million in tobacco use funds in the recent budget, implemented free school meals, allowing WIC to be used at local farmers markets and delivering food support to low-income families during the pandemic, Ogden said.
“More broadly, the Maine CDC’s effort to rebuild a regional approach to public health — which was dismantled under the LePage administration — will allow us to target funding toward community-based organizations that, in turn, will allow them to deploy solutions that work best for their communities to improve health outcomes. It is another example of the governor’s continued commitment to improving Maine’s public health system,” Ogden said.
Joanne Joy, senior program manager of prevention for Healthy Communities of the Capital Area, said she was concerned when Mills came into office that prevention didn’t appear to be a priority and it took a while to refill positions at the Maine CDC. There seemed to be more emphasis on healthcare than prevention, Joy said.
But overall the Mills administration has a broader view of keeping people healthy, said Joy, who has worked on obesity, tobacco use and substance prevention since 2001.
“My concern with a LePage administration is just his history,” Joy said. “His history was that the Maine CDC did not apply for every federal grant that they were qualified for. … It goes along with the philosophy of smaller government. When there’s smaller government, there’s smaller public health.”
While some health statistics continued to worsen under Mills, Joy said it is impossible to compare the last couple years during the pandemic to the LePage years.
“It’s impossible to say ‘setting aside COVID,’ because COVID permeated health, mental health, substance use. It just permeated it all. It just changed it all,” she said.
“It’s not apples to apples at all. It’s COVID and COVID and COVID.”
This story was originally published by The Maine Monitor, a nonprofit and nonpartisan news organization. To get regular coverage from the Monitor, sign up for a free Monitor newsletter here.



